Anthem Blue Cross and Blue Shield for Therapy
Anthem Blue Cross and Blue Shield plans is one of the largest health insurance companies in the country, with plans offered across multiple states. As a subsidiary of Blue Cross Blue Shield, Anthem Blue Cross and Blue Shield has an incredibly expansive provider network — which includes many excellent therapists.

Does Anthem Blue Cross and Blue Shield cover therapy?
Yes, Anthem Blue Cross and Blue Shield does cover therapy services. However, the amount of the therapy cost they cover depends on your unique health insurance plan. Because Anthem Blue Cross and Blue Shield is such a large health insurance company, they offer many different types of plans across their various geographies. This means that coverage for outpatient mental health services also varies widely.
However, Anthem Blue Cross and Blue Shield is dedicated to whole-person health, which includes mental health care. For this reason, they provide coverage across the majority of their health insurance plans.
How do I check if my Anthem Blue Cross and Blue Shield plan covers therapy?
To check if your Anthem Blue Cross and Blue Shield health insurance plan covers therapy services, head over to your Summary and Benefits document. You’ll likely find this document through your online Anthem Blue Cross and Blue Shield account. Within this document, you’ll find the different rates of coverage — including copayment or coinsurance amounts — for each type of service available. Look for “outpatient mental health services” to see your coverage for therapy.
Here is an example of what your Anthem Blue Cross and Blue Shield Summary of Benefits may look like, and where to find the Outpatient Mental Health line item:
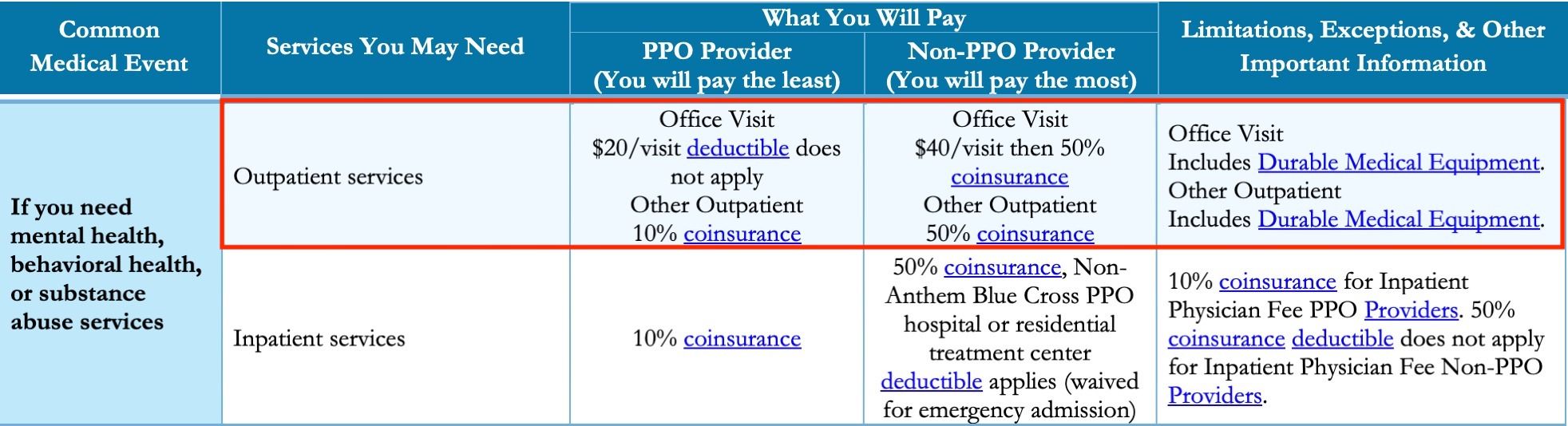
If your Summary and Benefits document does not share this information with you, give the phone number on the back of your insurance card a call. The Anthem Blue Cross and Blue Shield customer service department will share with you the coverage available to you through your plan.
How much does therapy cost with the Anthem Blue Cross and Blue Shield plan?
Because Anthem Blue Cross and Blue Shield offers so many health insurance plans, how much a person will pay for therapy out of their own pocket varies depending on their plan, their geography, and the therapist they see.
Anthem Blue Cross and Blue Shield only provides coverage for in-network therapists. This means that there is a set network of therapy providers to choose from — anyone else outside of this network will not be eligible for reimbursement. For this reason, it is typically most cost-effective to see an in-network therapist if you have Anthem Blue Cross and Blue Shield.
Many Anthem Blue Cross and Blue Shield health insurance plans require the client to pay a copayment that may be between $15-30 each session. Other plans require that the client pays a coinsurance, which may range from 20-80%. To find out your actual out-of-pocket expense for therapy, search your Summary and Benefits document for your plan’s rates.
What types of mental health conditions does Anthem Blue Cross and Blue Shield cover?
Anthem Blue Cross and Blue Shield covers many mental health conditions. To reimburse therapists or clients, Anthem Blue Cross and Blue Shield requires that the client receive a diagnosis from their therapist. This diagnosis guides treatment and insurance coverage.
Examples of eligible mental health conditions include:
- Depression
- Anxiety and stress
- Alcohol abuse
- Infertility concerns
- Grief and loss
- Eating disorders
- Learning disabilities
There are many more diagnosable — and reimbursable — mental health conditions, all of which Anthem Blue Cross and Blue Shield covers.
What types of therapy does Anthem Blue Cross and Blue Shield cover?
Anthem Blue Cross and Blue Shield covers many different types of therapy. As long as the therapist provides an evidence-based, clinically rigorous therapy modality that is appropriate for the given diagnosis, Anthem Blue Cross and Blue Shield will provide coverage.
These evidence-based therapy modalities include:
- Cognitive Behavioral Therapy (CBT)
- Dialectical Behavioral Therapy (DBT)
- Eye Movement Desensitization and Reprocessing (EMDR)
- Mindfulness practices
- Child-parent psychotherapy
- Acceptance and Commitment Therapy (ACT)
What types of therapy does Anthem Blue Cross and Blue Shield NOT cover?
Anthem Blue Cross and Blue Shield does not cover life coaching, career counseling, or holistic treatment modalities like aromatherapy, massage therapy, or non-medically required acupuncture. It also does not cover energy work such as reiki healing.
Anthem Blue Cross and Blue Shield requires therapists to be professionally credentialed and offering evidence-based treatment appropriate for the diagnosis.
Does Anthem Blue Cross and Blue Shield cover online therapy?
Yes, Anthem Blue Cross and Blue Shield offers coverage for online therapy. This opens the doors for many clients who aren’t able to physically attend therapy sessions each week. Anthem Blue Cross and Blue Shield even created their own online teletherapy resource center, LiveHealth Online, back in 2016, which is available in certain geographies.
Your coverage for therapy costs will remain the same, whether you visit your therapy in-person or online.
Does Anthem Blue Cross and Blue Shield cover couples therapy?
Whether Anthem Blue Cross and Blue Shield covers couples counseling depends on the plan. Generally, health insurance plans do not cover couples therapy. This is partially because there cannot be a diagnosis to base the reimbursement upon. However, some Anthem Blue Cross and Blue Shield plans may provide coverage at the same or differing rates as individual therapy. To see if yours does, visit your Summary and Benefits document.
However, many couples still benefit from seeing a therapist together. If your Anthem Blue Cross and Blue Shield health insurance plan does not include a couples counseling benefit, there may be ways to decrease the cost of couples counseling, such as sliding scale.
Do I need to see my primary doctor before starting therapy?
If your Anthem Blue Cross and Blue Shield health insurance plan is an HMO plan, you will need to get a referral from your primary care physician before you start seeing a therapist. This means that you’ll likely need to first schedule a visit with your primary care physician to get this referral.
However, some people have Anthem Blue Cross and Blue Shield PPO plans instead. If you have a PPO plan, you do not need a referral from your primary care physician before seeing a therapist. This means you can begin your search and mental health journey when you’re ready!
Find vetted therapists who are in-network with Anthem Blue Cross and Blue Shield
- Alabama
- Arizona
- Arkansas
- California
- Colorado
- Connecticut
- Delaware
- Florida
- Georgia
- Hawaii
- Idaho
- Illinois
- Indiana
- Iowa
- Kansas
- Kentucky
- Louisiana
- Maine
- Maryland
- Massachusetts
- Michigan
- Minnesota
- Mississippi
- Missouri
- Montana
- Nebraska
- Nevada
- New Hampshire
- New Jersey
- New Mexico
- New York
- North Carolina
- North Dakota
- Ohio
- Oklahoma
- Oregon
- Pennsylvania
- Rhode Island
- South Carolina
- South Dakota
- Tennessee
- Texas
- Utah
- Vermont
- Virginia
- Washington
- Washington DC
- West Virginia
- Wisconsin
- Wyoming