Magellan Health for Therapy
Magellan Health is a healthcare company that specializes in behavioral health benefits. Many health insurance companies partner with Magellan Health to provide members with access to therapy services from an expansive provider network. This means that many of its members have a health insurance plan with another health insurance company but receive mental health services through Magellan Health.

Does Magellan Health cover therapy?
Yes, Magellan Health provides therapy coverage for its members. Magellan Health offers members a choice of many different plans, so be sure to check the details of your specific plan to learn more about your mental health coverage.
How do I check if my Magellan Health plan covers therapy?
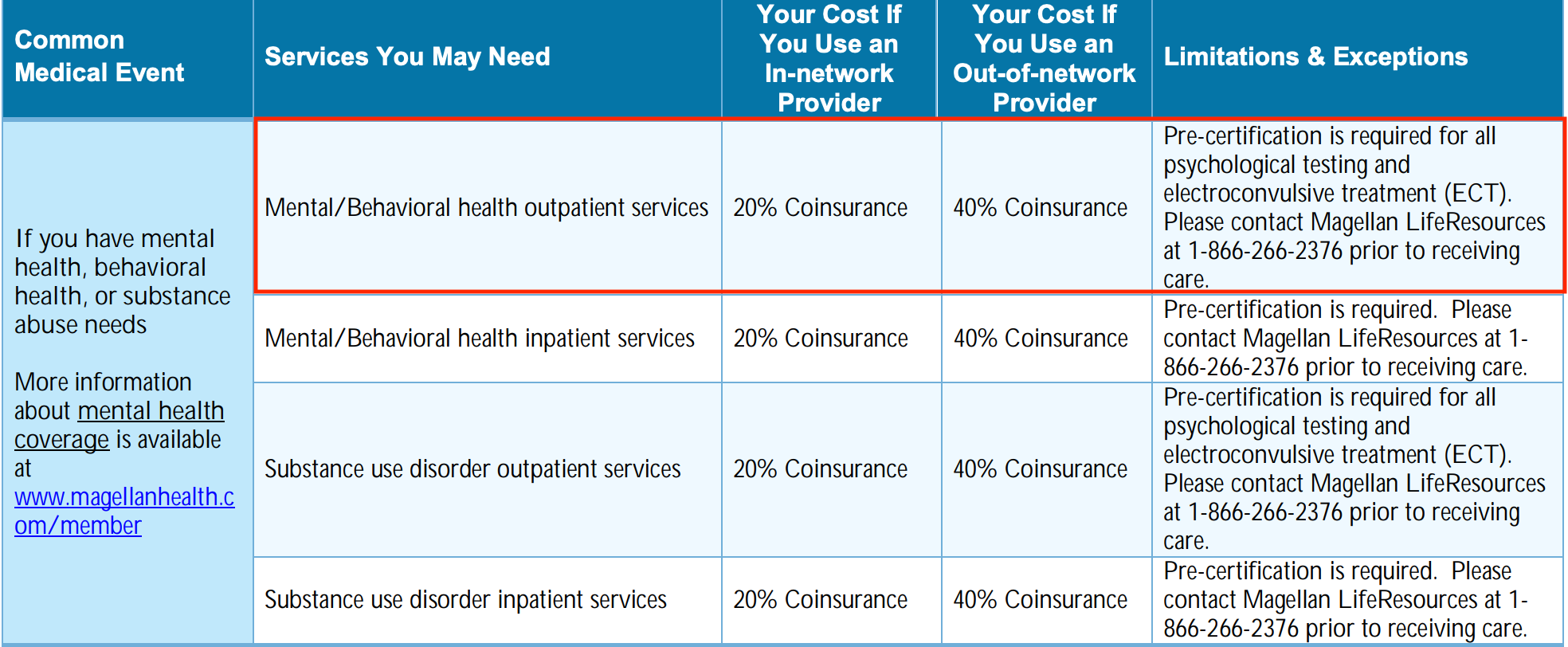
To check if your Magellan Health plan covers therapy, find your Summary and Benefits document. This document is a list of how much your Magellan Health plan covers and how much of the costs will be your responsibility — look under “outpatient mental health” or “mental/behavioral health outpatient services” to find this item. You can usually find your Summary and Benefits document through your Magellan Health online portal.
You can also call the Magellan Health customer service hotline to speak with a representative to learn more about your plan’s mental health benefits. Find this number on the back of your insurance card and ask about therapy costs.
How much does therapy cost with my Magellan Health plan?
While the cost for therapy depends on your Magellan Health plan, expect to pay a coinsurance of 20 - 40% per session with your in-network therapist. This means that you’ll typically pay a 20 - 40% of the overall therapy cost and Magellan Health will pay the rest.
This cost will rise when you choose to see an out-of-network therapist. Costs will also vary based on your primary health insurance plan.
What types of mental health conditions does Magellan Health cover?
Magellan Health insurance covers services for many mental health conditions. To reimburse therapists or clients, Magellan Health requires that the client receive a diagnosis from their therapist. This diagnosis guides treatment and the insurance coverage.
A few possible mental health conditions covered by Magellan Health include:
What types of therapy does Magellan Health cover?
Magellan Health requires that a licensed therapist provide evidence-based, clinically rigorous therapy to be eligible for reimbursement.
These evidence-based therapy modalities include:
- Cognitive Behavioral Therapy (CBT)
- Dialectical Behavioral Therapy (DBT)
- Eye Movement Desensitization and Reprocessing (EMDR)
- Mindfulness practices
- Child-parent psychotherapy
- Acceptance and Commitment Therapy (ACT)
There are many more types of therapies — and often, therapists blend modalities into their own approaches, all of which are covered by Magellan Health.
What types of therapy does Magellan Health NOT cover?
Magellan Health does not cover life coaching or career counseling — this is because coaching is generally based upon goals rather than a diagnosis. Magellan Health also does not provide coverage for holistic treatment modalities like aromatherapy or massage therapy. It does not cover energy work such as reiki healing.
Does Magellan Health cover online therapy?
Yes, Magellan Health covers online therapy. Clients have the option of seeing their Magellan Health provider online or in-person, with the same coverage rates and benefits. Many clients find that seeing a therapist online, rather than in-person, is convenient and more accessible.
Does Magellan Health cover couples therapy?
Some Magellan Health plans cover couples therapy — so it’s important to check your specific Magellan Health plan to see if you have a couples therapy benefit. You may find coverage by seeing your individual therapist with your partner or partners. There are also many ways to make couples therapy more affordable, in the event that your Magellan Health plan does not cover couples therapy.
Do I need to see my primary doctor before starting therapy?
Because Magellan Health contracts with various health insurance companies to provide behavioral health services, it will depend on your health insurance plan whether or not you need a referral from your primary care physician before beginning your search for a great therapist. If you have an HMO health insurance plan, you will need to see your primary care physician before you start therapy. However, if you have a PPO health insurance plan, you can start to look for a therapist that matches your needs as soon as you’re ready.
Find vetted therapists who are in-network with Magellan Health
- Alaska
- Arizona
- Arkansas
- California
- Colorado
- Connecticut
- Delaware
- Florida
- Georgia
- Hawaii
- Illinois
- Indiana
- Kansas
- Kentucky
- Louisiana
- Maine
- Maryland
- Massachusetts
- Michigan
- Minnesota
- Nevada
- New Hampshire
- New Jersey
- New Mexico
- New York
- North Carolina
- Ohio
- Oregon
- Pennsylvania
- Rhode Island
- South Carolina
- Texas
- Utah
- Vermont
- Virginia
- Washington
- Washington DC
- West Virginia
- Wisconsin