Emblem Health for Mental Health Coverage
EmblemHealth is a large health insurance company that insures over 3 million residents of the East Coast. They began with a strong focus on community health in New York City and from that background, they’ve kept their dedication to providing mental health services for their members — including therapy! EmblemHealth insurance administers plans for individuals, families, companies of all sizes, as well as Medicare and Medicaid plans.

Does EmblemHealth cover therapy?
Yes, EmblemHealth covers behavioral and mental health services, including substance abuse treatment and intensive outpatient programs, within their provider network. They have an expansive network of mental health professionals across the tristate area that form their in-network provider group.
EmblemHealth covered treatment depends on the plan that you have. Many EmblemHealth plans cover a part of the treatment services fees but not all of it. Many EmblemHealth participants are required to pay a copayment for each session with a therapist.
EmblemHealth does not cover therapy services with providers outside of their network — there are no out-of-network benefits, which means that members who hope to begin therapy will typically find it most cost-effective to work with a therapist in-network with EmblemHealth in New York, New Jersey, and Connecticut.
How do I check if my EmblemHealth plan covers therapy?
To check if your EmblemHealth plan covers therapy, read your Summary and Benefits document. Look for the line that includes “outpatient mental health care.” This line will tell you the amount of the session fee for which you’ll be responsible.
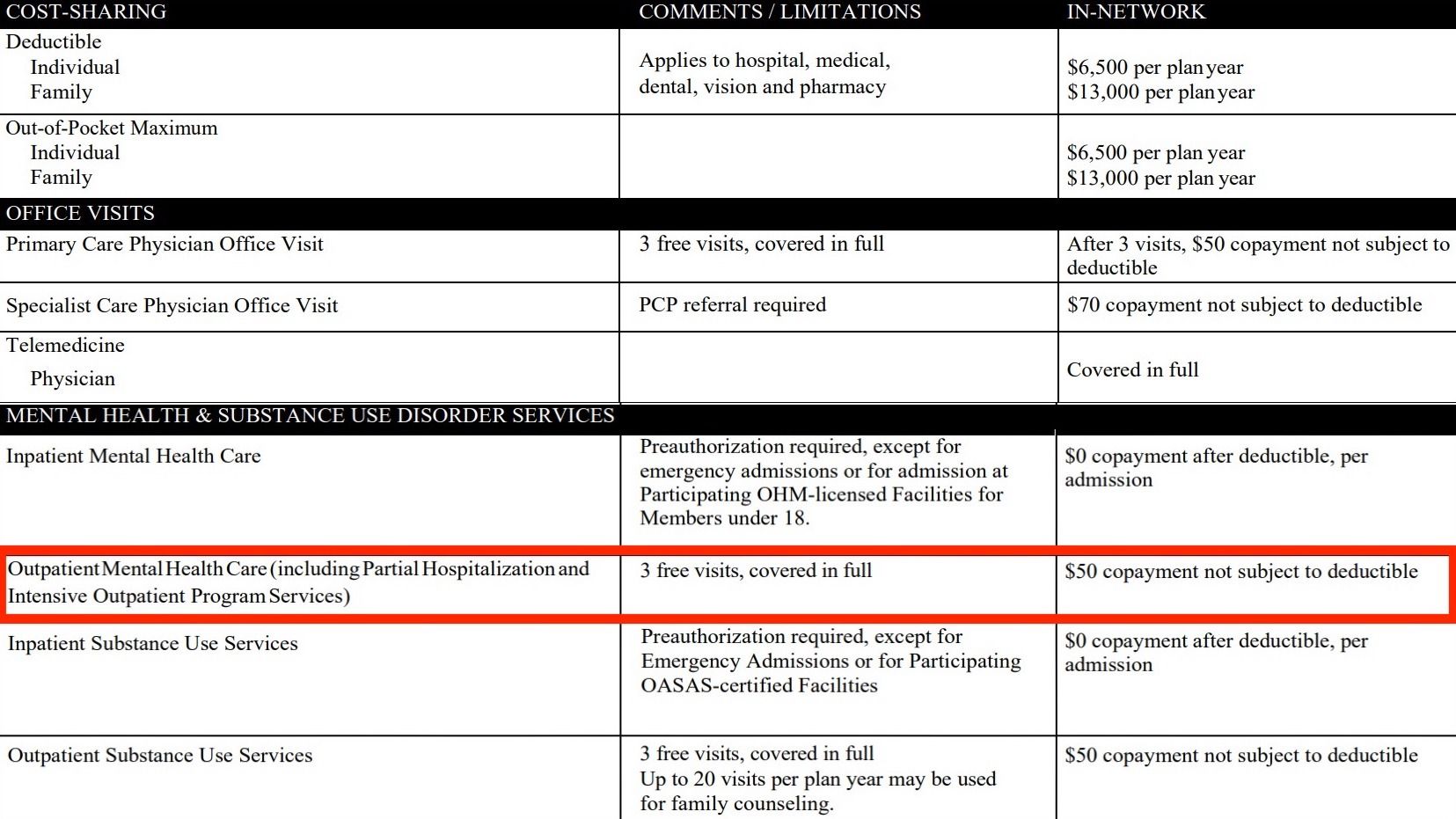
Generally, insurance companies post the Summary and Benefits document within their online portals. If you’re not able to locate this document, find the customer service number on the back of your insurance card. The customer service agent will either point you in the right direction of where to find your mental health benefits or share with you the amount of provided health coverage you have under your plan.
How much does therapy cost with the EmblemHealth plan?
Across most EmblemHealth plans, expect to pay around $50 each therapy session for in-network providers. This means that each time that you have a healthcare service or therapy session, you will pay your therapist $50 out-of-pocket. This cost does not account towards your insurance coverage deductible.
The cost of therapy under EmblemHealth varies based on the participant’s enrollment. EmblemHealth offers many different plan options, including employer-sponsored, Medicare, and Medicaid plans. On top of this, they have HMO plans as well as PPO plans. Because EmblemHealth insurance covers more than one state, your plan will also vary by your location, whether you’re in New York or elsewhere in the tristate area. All these factors contribute to a wide range of therapy coverage.
If you see a therapist who is not a member of the EmblemHealth provider network, you will not have coverage and should expect to pay the full session cost out-of-pocket. This could range from $50 - $250 or more. This could be substantial based on location as therapists and medical centers in New York tend to be more expensive than other locations.
If you’re concerned about paying for therapy, ask your therapist about sliding scale options. If your therapist offers sliding scale payments, you may be eligible to pay a lowered fee per session.
What types of mental health conditions does EmblemHealth cover?
EmblemHealth mental health benefits include treatment services for the following mental health disorders, as well as substance abuse disorder(s), and more:
- Depression
- Anxiety
- Alcohol abuse
- Drug abuse
- Grief and loss
- Eating disorders
- Obsessive compulsive disorder (OCD)
When you start therapy with an in-network therapist, they will appoint a diagnosis for your condition or goals. They’ll share this diagnosis with the insurance company to ensure coverage. This is essential for coverage of your therapy sessions or addiction treatment services. It is not uncommon for one diagnosis to have a co-occurring disorder, for instance, depression and substance abuse.
If you would prefer that your therapist doesn’t disclose your diagnosis with your health insurer, consider your out-of-network options. This way, your mental health care stays between you and your therapist — not the insurance company and anyone who has access to your insurance account information.
What types of treatment does EmblemHealth cover?
EmblemHealth covers many different evidence-based therapy approaches and modalities. This includes but is not limited to:
- Cognitive Behavioral Therapy (CBT)
- Dialectical Behavioral Therapy (DBT)
- Eye Movement Desensitization and Reprocessing (EMDR)
- Mindfulness practices
- Psychodynamic therapy
- Acceptance and Commitment Therapy (ACT)
In order to provide coverage for treatment, EmblemHealth requires that therapists perform diagnosis-based therapy appropriate for mental health diagnosis. Many therapists blend their approaches while meeting with clients. As long as the therapist meets all of the EmblemHealth requirements, they are eligible for reimbursement.
Additionally, EmblemHealth has coverage for substance abuse and addiction treatment that ranges from outpatient partial hospitalization programs to inpatient programs that require a higher intensity treatment setting. Generally, a person seeking treatment in a partial hospitalization program or residential programs for addiction treatment or eating disorders will need a referral from a primary care physician.
What types of therapy does EmblemHealth NOT cover?
If a therapy approach is not evidence-based — that is, has empirical research backing its efficacy — EmblemHealth will not cover therapy costs.
This includes life coaching and career coaching, as these disciplines use the same therapies and modalities, they are less based on mental health literature and more on goal setting and achievement. EmblemHealth does not cover holistic approaches to treatment such as aromatherapy, massage therapy, or nutritional therapy. They also do not cover hypnosis, ketamine, and psychedelic treatments, even if the purpose of this treatment is for substance abuse treatment or a mental health condition.
Does EmblemHealth cover online therapy?
Yes, online therapy is covered. As more therapists offer both in-person and online options, EmblemHealth recognizes the importance of accessible mental health treatment. While EmblemHealth may require the therapist to follow certain policies — such as using a secure video platform — clients can see their in-network therapists online instead of in the office or treatment center without a change in their cost. This means that you’ll pay the same amount to see your therapist online as you would in-person.
Does EmblemHealth cover couples therapy?
Some plans offer coverage for couples counseling, but not all of them. One of the reasons for this is because there is no diagnosis within couples’ sessions, which makes the services ineligible for reimbursement.
However, some plans do have couples counseling as a benefit, and there are also many ways to make couples sessions more affordable. This opens the door for you and your partner or partners to work with a high-quality couples therapist and grow your relationships.
Do I need to see my primary care doctor before starting therapy?
Depending on your EmblemHealth insurance plan, you may need to receive a referral from your primary care physician before you begin seeing your therapist. For all EmblemHealth plans that are HMO, you will need to visit your primary care physician and share your interest in mental healthcare. This is a quick and common process that should not be a major roadblock in your therapy journey!
If you have a PPO or an EPO EmblemHealth plan, then you won’t need a referral before you begin therapy. You can start your search for a great fitting therapist when you’re ready!