Humana for Therapy
Humana is a large health insurance company that aims to support healthy lives across the lifespan. They provide health insurance coverage — through HMO, PPOs, FFS, and SNP plans — for millions of Americans across the country, which typically includes mental health benefits like therapy. Humana Behavioral Health is a subsidiary of Humana and is the company responsible for offering therapy coverage for its members through the management of a therapist network.

Does Humana cover therapy?
Yes, Humana health insurance plans offer therapy coverage. While Humana is a sizable health insurance company that offers dozens of plans, all of their plans have mental health benefits. The amount of coverage, however, depends on your location, your therapist’s provider status, and your exact plan type.
Humana Behavioral Health, the arm of the health insurance company that provides mental health benefits, includes a team of care managers to help you understand your benefits and guide you in your search for a budget-friendly therapist.
How do I check if my Humana plan covers therapy?
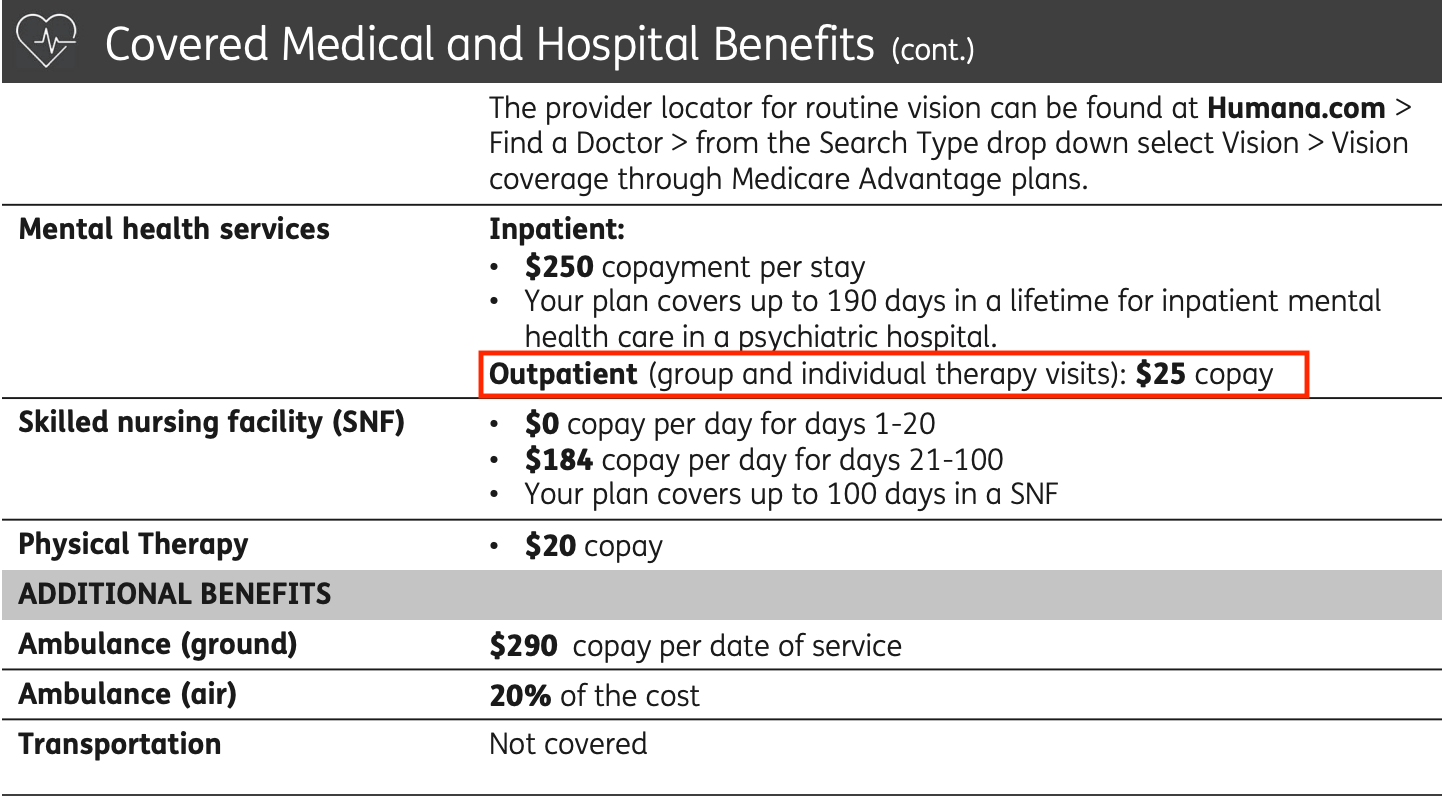
Each Humana plan comes with its own Summary and Benefits document. The Summary and Benefits document lists out the coverage provided for each service type, usually in a line-by-line format. This makes it easy for you to figure out how much therapy coverage your Humana plans allows — and to calculate how much therapy will cost you. When you find your Summary and Benefits document, which is generally found online through your Humana portal, look for the “mental health services” line. There, you’ll find the coverage rates for both in-network and out-of-network therapy visits.
You might also call the phone number on the back of your Humana health insurance card to learn more about your specific plan details and mental health benefits coverage. You’ll speak with a Humana customer service representative who can answer your questions.
How much does therapy cost with my Humana plan?
While therapy costs depend on your specific plan, expect to pay a copayment of between $25 - $100 per visit with your in-network therapist. Some plans offer coverage for out-of-network therapists as well, ranging from 25% - 45% coinsurance, which means that you’ll be responsible for that amount of the session fee each time you see your therapist. It’s typically most cost-effective to see a therapist in-network with Humana.
If you’re concerned about the cost of therapy, there are many ways to decrease the impact on your budget such as sliding scale fees or joining a support group.
What types of mental health conditions does Humana cover?
Boosting mental health is part of the Humana mission. From that mission, Humana provides coverage for a wide range of mental health conditions. These conditions include:
When you start therapy, your therapist will designate a diagnosis for your condition, situation, or goals. They’ll share this diagnosis with Humana as a way of accounting for coverage. If you would prefer that your therapist doesn’t disclose your diagnosis with Humana, consider your out-of-network options. This way, your mental health care stays between you and your therapist — not the insurance company and anyone who has access to your insurance account information.
What types of therapy does Humana cover?
It’s important and vital to Humana that all mental healthcare is based on evidence, clinical rigor, and the given diagnosis. This is a way of ensuring appropriate care and reimbursement for each of its members. They provide coverage for all therapy modalities proven to reach healthy and desired outcomes, including:
- Cognitive Behavioral Therapy (CBT)
- Dialectical Behavioral Therapy (DBT)
- Eye Movement Desensitization and Reprocessing (EMDR)
- Mindfulness practices
- Psychodynamic
- Acceptance and Commitment Therapy (ACT)
Often, therapists use blended methods as they individualize treatment for each client. As long as the therapist is professionally credentialed and provides appropriate therapeutic services, Humana will cover therapy sessions.
What types of therapy does Humana NOT cover?
If a therapy approach is not evidence-based — that is, it lacks empirical research backing its efficacy — Humana will not cover therapy costs.
This includes life coaching and career coaching, as these disciplines are less based on mental health diagnosis and more on goal-setting and achievement. Humana does not cover holistic approaches to treatment such as aromatherapy, massage therapy, or nutritional therapy. They also do not cover ketamine and psychedelic treatments, even if the purpose of this treatment is for a mental health condition. Humana does not cover energy work such as reiki healing.
Does Humana cover online therapy?
Yes, Humana provides coverage for online therapy and telehealth. They approved coverage for online visits with providers during the pandemic, so while unlikely, Humana may rescind this policy in the future. If you would like to see your therapist online rather than in-person, check with your Humana benefits to make sure that you understand your online coverage.
Generally, health insurance companies provide the same amount of coverage for all visit types, both in-person and online. This means that you’ll have the same copayments and coinsurance rates if you see your therapist through a virtual platform as if you saw them at their office.
Does Humana cover couples therapy?
Some Humana health insurance plans may provide coverage for couples therapy, however the majority of health insurance plans do not offer this as a benefit. This is in part because it is difficult for the therapist to bill for reimbursement under the required mental health condition diagnosis. Check with your specific Humana health insurance plan to learn more about your couples therapy coverage.
If you’re still interested in couples therapy, there are many ways to make it more affordable. This opens the door for you and your partner or partners to work with a high-quality couples therapist and grow your relationships.
Do I need to see my primary doctor before starting therapy?
You may need to see your primary care physician before starting therapy if you have an HMO plan. HMO health insurance plans require that the member attain a referral for mental healthcare before seeing a therapist.
If your plan is a PPO or FFS plan, you will not need to see your primary care physician before finding a great therapist — you can start your search for the right therapist for you whenever you’re ready.
Find vetted therapists who are in-network with Humana
- Alabama
- Alaska
- Arizona
- Arkansas
- California
- Colorado
- Connecticut
- Delaware
- Florida
- Georgia
- Hawaii
- Idaho
- Illinois
- Indiana
- Iowa
- Kansas
- Kentucky
- Louisiana
- Maine
- Maryland
- Massachusetts
- Michigan
- Minnesota
- Mississippi
- Missouri
- Montana
- Nebraska
- Nevada
- New Hampshire
- New Jersey
- New Mexico
- New York
- North Carolina
- North Dakota
- Ohio
- Oklahoma
- Oregon
- Pennsylvania
- Rhode Island
- South Carolina
- South Dakota
- Tennessee
- Texas
- Utah
- Vermont
- Virginia
- Washington
- Washington DC
- West Virginia
- Wisconsin
- Wyoming